Research
Can a Bone Density Test Reveal Arthritis?
Are you curious if a bone density test can reveal indicators of arthritis? Those who are concerned about their bone health frequently ask this question. A bone density test is commonly used to identify osteoporosis, however it is not the major diagnostic technique for arthritis.
Arthritis is a disorder that causes joint inflammation and pain. A bone density test assesses bone strength and density but does not directly diagnose arthritis. However, it can help rule out other illnesses or issues that may have an impact on bone health.
Doctors often use a combination of variables to diagnose arthritis, including a physical examination, medical history, imaging tests such as X-rays or MRIs, and blood tests to detect specific inflammation markers.
Understanding Bone Density Tests
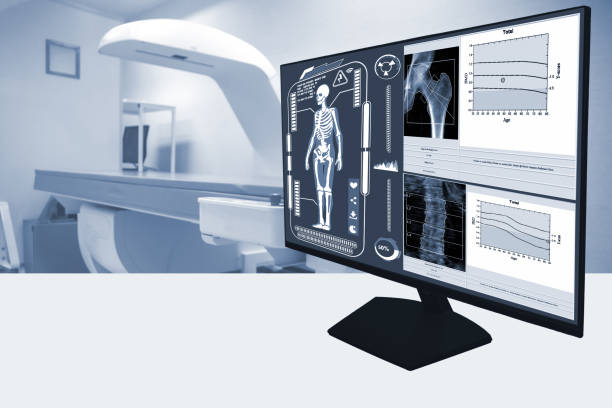
Bone density tests, often called dual-energy X-ray absorptiometry (DXA or DEXA) scans, are routinely used to assess bone strength and density. The test uses a low-dose X-ray that goes through the bones and measures the quantity of radiation absorbed. This test indicates the bone mineral density (BMD), which is an important element in assessing bone health.
A bone density test involves the patient lying on a table while a scanner moves over the body, typically focused on the hip, spine, or forearm. The results are often reported as a T-score, which compares the patient’s BMD to that of a healthy young adult of the same gender. A T-score of -1 or higher is considered normal, a T-score of -1 to -2.5 shows poor bone mass (osteopenia), and a T-score of -2.5 or lower suggests osteoporosis.
While bone density tests are useful for diagnosing osteoporosis, they have limits in detecting other bone-related disorders such arthritis. Arthritis typically affects the joints, which cannot be readily measured by a bone density test.
What is Arthritis and How is it Diagnosed?
Arthritis is a broad word that refers to more than 100 distinct disorders affecting the joints and surrounding tissues. The most prevalent types of arthritis are osteoarthritis, rheumatoid arthritis, and psoriatic arthritis.
Healthcare practitioners evaluate a number of factors when determining an arthritis diagnosis. These may involve a physical examination to determine joint discomfort, edema, and range of motion. In addition, they will consider the patient’s medical history, particularly any family history of arthritis or other autoimmune disorders. Imaging studies, such as X-rays and MRIs, can also provide useful information on joint injury, inflammation, and anomalies.
C-reactive protein (CRP) and rheumatoid factor (RF) are two examples of inflammation markers that are frequently detected by blood tests. These tests can help distinguish between different types of arthritis and rule out other illnesses that present similar symptoms.
It’s crucial to note that arthritis is a complex ailment that frequently need the consultation of a rheumatologist. They will make an accurate diagnosis based on the patient’s symptoms, medical history, and test results.
Can a Bone Density Test Detect Arthritis?
While a bone density test is useful for measuring bone health, it does not directly diagnose arthritis. A bone density test is primarily used to assess fracture risk and diagnose osteoporosis. However, it can indirectly provide some information about the impact of arthritis on bone health.
Arthritis can cause changes in bone density over time. In some situations, arthritis-related chronic inflammation can induce bone loss, resulting in decreased bone mineral density. This can raise the risk of fractures in people with arthritis, especially if they also have other risk factors like age or low body weight.
However, increases in bone density alone are insufficient for diagnosing arthritis. Other diagnostic procedures, including as imaging tests and blood tests, are required to confirm the presence of arthritis and identify the type of arthritis afflicting the patient.
Individuals with arthritis may benefit from a bone density test to examine their overall bone health and discover any extra fracture risk factors. However, it should not be used alone to diagnose arthritis.
Limitations of Bone Density Tests in Detecting Arthritis
While bone density scans are useful for identifying osteoporosis, they are limited in their ability to diagnose arthritis. As previously stated, arthritis predominantly affects the joints, which cannot be easily examined with a bone density test.
Arthritis is a complex disorder that causes joint inflammation, cartilage loss, and other structural abnormalities. These alterations do not usually show up in bone density measures. Furthermore, many types of arthritis, such as rheumatoid arthritis, can produce joint swelling and inflammation without significantly affecting bone density.
It’s critical to understand that a bone density test is only one piece of the puzzle when it comes to evaluating bone health and diagnosing arthritis. Other diagnostic procedures, including as imaging and blood testing, are required to offer a thorough assessment of joint health and confirm the existence of arthritis.
Other Diagnostic Methods for Arthritis
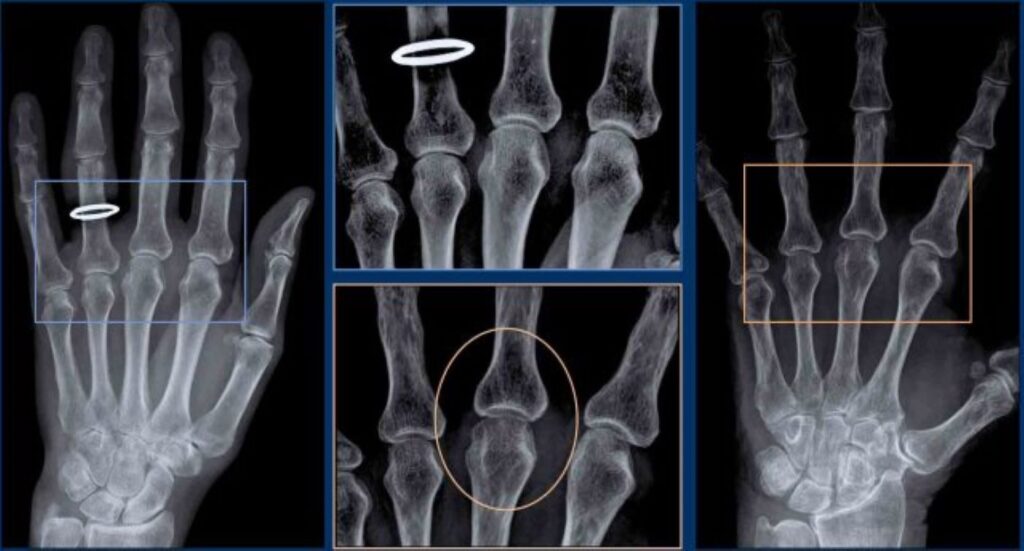
To effectively diagnose arthritis, healthcare practitioners employ a variety of diagnostic procedures. In addition to a physical exam, they may request imaging tests, such as X-rays, MRIs, or ultrasound scans, to see the joints and diagnose any damage or abnormalities.
X-rays are routinely used to diagnose joint deterioration, such as joint constriction or bone spurs. MRIs produce detailed images of soft tissues, such as the cartilage and ligaments that surround the joints. Ultrasound scans can assess joint inflammation, fluid collection, and the presence of synovitis, which is inflammation of the synovial membrane that lines the joints.
Blood tests are also necessary for determining the diagnosis of arthritis. They can assist in detecting inflammatory signs such as increased C-reactive protein (CRP) or erythrocyte sedimentation rate. Specific antibody tests, such as rheumatoid factor (RF) or anti-cyclic citrullinated peptide (anti-CCP) antibodies, are also used to detect several kinds of arthritis, including rheumatoid arthritis.
By combining the results of these many diagnostic tools, healthcare practitioners can make an accurate diagnosis and create a suitable treatment plan for arthritis patients.
The Link Between Bone Density and Arthritis
While a bone density test is not a diagnostic tool for arthritis, there is a correlation between bone density and how arthritis affects bone health. Arthritis can cause changes in bone density over time, owing to persistent inflammation and other variables related with the condition.
Inflammatory arthritis, such as rheumatoid arthritis, can lead to bone loss and decreased mineral density. Chronic inflammation in the joints can cause accelerated bone resorption, which occurs when bone tissue breaks down quicker than it is replaced. Over time, this can lead to decreased bone density and a higher risk of fractures.
Individuals with arthritis should focus on maintaining good bone health to reduce their risk of fractures. This includes eating a well-balanced diet high in calcium and vitamin D, doing regular weight-bearing activities, and avoiding smoking and excessive alcohol intake. In addition, healthcare providers may prescribe medicine to reduce inflammation and protect bone health.
Regular bone density testing, such as DXA scans, can help follow changes in bone health over time and inform treatment options for people with arthritis.
Importance of Early Detection and Treatment for Arthritis
Early detection and adequate management are critical for reducing the impact of arthritis on a person’s quality of life. The sooner arthritis is recognized, the sooner proper therapy can begin to alleviate symptoms, halt disease progression, and avoid joint injury.
Delaying diagnosis and treatment may result in more severe joint injury and irreversible alterations. Early intervention can help people with arthritis retain joint function, reduce pain and inflammation, and enhance their overall quality of life.
If you feel you have arthritis, you should speak with a rheumatologist. They can assess your symptoms, do the required diagnostic tests, and create a personalized treatment plan based on your individual requirements.
Remember that everyone’s arthritis experience is unique, and treatment options may vary. Working closely with a healthcare professional will ensure you receive the best possible care for your condition.

Managing Arthritis Through Lifestyle Changes and Medication
While there is no cure for arthritis, there are numerous treatment options that can help control symptoms and improve quality of life. Arthritis treatment frequently includes lifestyle modifications, medication, and other therapeutic measures.
Lifestyle changes can have a substantial impact on arthritis treatment. Maintaining a healthy weight can assist to relieve stress on the joints, particularly weight-bearing joints like the knees and hips. Regular exercise, which includes both aerobic and strength training, can improve joint flexibility, strengthen muscles, and relieve pain and stiffness.
A well-balanced diet high in fruits and vegetables, whole grains, lean meats, and healthy fats can improve general health and minimize inflammation. Omega-3 fatty acids, found in fatty fish such as salmon or in supplements, may have anti-inflammatory qualities that can help people with arthritis.
In addition to lifestyle adjustments, medication is frequently used to treat arthritic symptoms and delay disease progression. NSAIDs can help alleviate pain and inflammation. Individuals with inflammatory forms of arthritis may be offered disease-modifying antirheumatic medications (DMARDs) and biologic medicines in order to regulate disease activity and protect joints.
It is critical to collaborate closely with a healthcare practitioner to determine the best treatment option for your individual form of arthritis. They can assist in selecting the appropriate drug, monitoring its effectiveness, and managing any potential side effects.
Conclusion
While a bone density test is not the primary diagnostic technique for arthritis, it is useful in assessing general bone health and determining the risk of fractures, particularly in people with arthritis. Changes in bone density can come from chronic inflammation and other arthritis-related causes.
However, a bone density test alone is insufficient to detect arthritis. Healthcare practitioners use a variety of elements to accurately diagnose arthritis, including physical examinations, medical histories, imaging studies, blood testing, and other diagnostic tools.
If you feel you have arthritis, you should speak with a rheumatologist. They can assess your symptoms, do the required diagnostic tests, and create a personalized treatment plan based on your individual requirements.
Trusted Health, Wellness, and Medical advice for your well-being